Antibodies for Studying Th1, Th2, and Th17 Cells
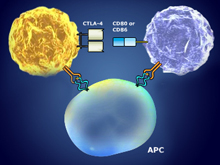
Th1 Cells and Molecules
Type 1 CD4+ T effector cells (Th1 cells) originate from naive T cells, which differentiate into Th1 cells by engaging STAT1, STAT4, and T-bet transcription factors. Th1 cells regulate the immune system by activating macrophages to destroy intracellular pathogens. This is achieved by the release of the proinflammatory cytokines, IL-2, LTa and IFN?. These cytokines are routinely used as a way of identifying Th1 cells and distinguishing them from similar cell types. Th1 cells have been associated with many autoimmune diseases, in particular multiple sclerosis and arthritis.
Th2 Cells and Molecules
Th2 cells are produced when the naive T cell receives a signal from IL-4 to engage STAT6 and GATA-3 transcription factors. Th2 cells secrete IL-4, IL-5 and IL-13 cytokines which results in the recruitment of immune effectors which eliminate extracellular parasites. Th2 cells are also known to have a fundamental role in allergic responses and have been implicated in diseases such as asthma.
Th17 Cells and Molecules
Th17 cells have only been discovered in recent years. They were assigned the name Th17 due to their ability to produce the proinflammatory cytokine IL-17A, and other molecules within this family. IL-17A signalling by Th17 cells triggers tissue inflammation which will in turn attract immune effector cells such as macrophages and granulocytes. Th17 cells are very distinct from other Th cell populations due to their release of IL-17, as this cytokine signaling is unique to Th17 cells. Like Th1 and Th2 cells, Th17 cells originate from naive T cells and become Th17 cells due to the activation of the transcription factors ROR?t and STAT3. Currently Th17 cells are being studied to determine if they are implicated in autoimmune disease.
Click on the links below to explore our product range through the various categories.
Further reading
-
Kurts, C (2008) Th17 cells: a third subset of CD4+ T effector cells involved in organ-specific autoimmunity.
Nephrol. Dial. Transplant. 23:816-819




